Depression, genetics, and why SSRIs may not be your thing
(You can suggest changes to this post.)
I’m currently consuming neuroscience papers like crazy as part of the talk I’m giving at OSCON tomorrow. I’m currently reading an excellent overview on serotonin transporters¹, and in particular looking at knock-out mice that can’t synthesize the serotonin transporter—the molecule which gets serotonin out of the synaptic cleft and back into neurons.
Mice lacking the transporter show a huge number of altered behaviours in line with depression and other mental illnesses in humans. They tend to have lots of serotonin sloshing around in their synaptic clefts (because it can’t get back into their neurons), and neurons which fire based upon serotonin signals appear to be less responsive (there’s much less clear “on-off” signalling).
Almost all our drugs for treating depression involve increasing the amount of serotonin and/or other monoamines (such as noradrenaline) in the synaptic cleft. But if you’re a knock-out mouse, you already have oodles of this stuff floating around there. We’re not sure if antidepressants alleviate the signs of depression in these mice, because giving them antidepressants increases serotonin to levels that are neurotoxic.
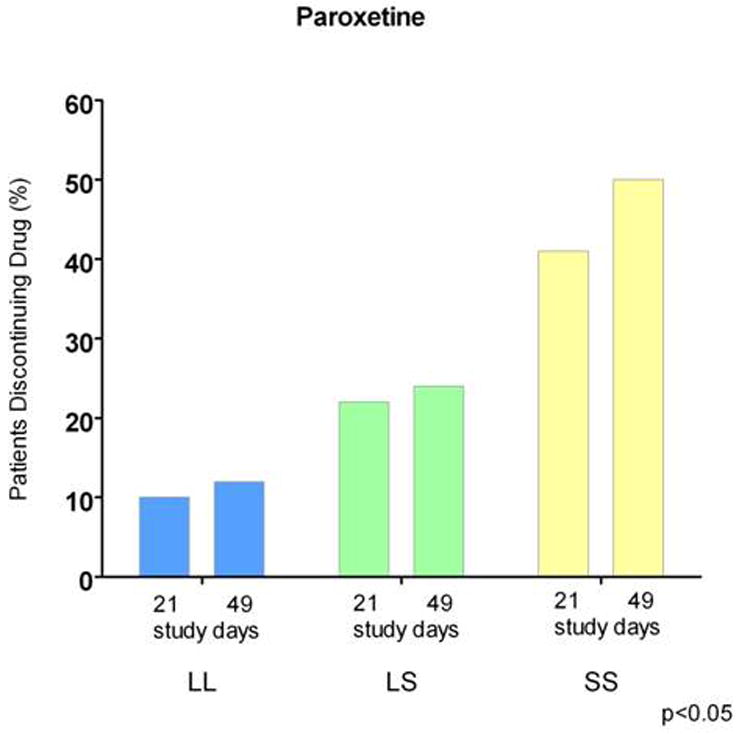
Humans show a polymorphism in the promoter region of the serotonin transporter gene. Those with short promoter regions appear to have less transporters produced, and they also show a significant aversion to continuing traditional anti-depressants. The theory is that treatment causes mild serotonin syndrome.
The more I research, the more it becomes immensely apparent that depression is not a disease, it’s not something with a single cause. It’s a syndrome. There’s a number of underlying pathologies, any of which can result in the state we know as “depression”. It’s no wonder that only about half of patients respond fully to treatment² (therapy AND drugs).
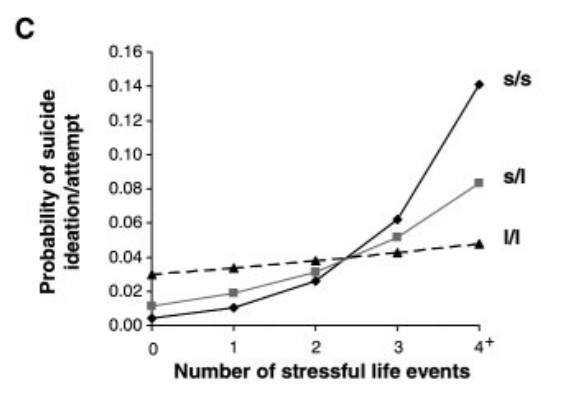
We know genetics explains about 50% of susceptibility to depression³, but there’s still this big 50% that isn’t explained. There’s a lot of evidence that’s pointing towards stress, and we think there might be something to do with Brain-Derived Neurotrophic Factor, but as a syndrome the involvement of stress and/or BDNF may be implicated in some cases of depression, but not others.
One thing that is certain is that depression absolutely sucks, and the more we’re able to understand the underlying causes and possible treatments, the better.
Edit: The next day I did indeed give a presentation on the neuroscience behind depression, along with my personal experiences. You can watch it online.
References
¹ Murphy, Dennis L., Meredith A. Fox, Kiara R. Timpano, Pablo R. Moya, Renee Ren-Patterson, Anne M. Andrews, Andrew Holmes, Klaus-Peter Lesch, and Jens R. Wendland. “How the Serotonin Story Is Being Rewritten by New Gene-based Discoveries Principally Related to SLC6A4, the Serotonin Transporter Gene, Which Functions to Influence All Cellular Serotonin Systems.” Neuropharmacology 55, no. 6 (2008): 932–960.
² Berton, Olivier, and Eric J. Nestler. “New Approaches to Antidepressant Drug Discovery: Beyond Monoamines.” Nature Reviews Neuroscience 7, no. 2 (2006): 137–151.
³ Kendler, Kenneth S., Ronald C. Kessler, Ellen E. Walters, Charles MacLean, Michael C. Neale, Andrew C. Heath, and Lindon J. Eaves. “Stressful Life Events, Genetic Liability, and Onset of an Episode of Major Depression in Women.” American Journal of Psychiatry 152, no. 6 (1995): 833–842.
⁴ Caspi, Avshalom, Karen Sugden, Terrie E. Moffitt, Alan Taylor, Ian W. Craig, HonaLee Harrington, Joseph McClay, Jonathan Mill, Judy Martin, and Antony Braithwaite. “Influence of Life Stress on Depression: Moderation by a Polymorphism in the 5-HTT Gene.” Science Signaling 301, no. 5631 (2003): 386.
3 Myths That Block Progress For The Poor
The belief that the world can’t solve extreme poverty and disease isn’t just mistaken. It is harmful. Read more...
 This site is ad-free, and all text, style, and code may be re-used under
a Creative Commons Attribution 3.0 license.
If like what I do, please consider
supporting me on Patreon,
or donating via Bitcoin (1P9iGHMiQwRrnZuA6USp5PNSuJrEcH411f).
This site is ad-free, and all text, style, and code may be re-used under
a Creative Commons Attribution 3.0 license.
If like what I do, please consider
supporting me on Patreon,
or donating via Bitcoin (1P9iGHMiQwRrnZuA6USp5PNSuJrEcH411f).
